Workers' Comp Referral & Case Management
The Problem
The Solution

Digital Intake
Start with a clean claim.
The wrong info up front causes downstream delays and rework. Hatch captures everything at the start so the rest runs smooth.
WC-specific digital intake forms
AI document processing
Review-and-confirm workflow
Partner Portal
Adjusters chew up hours each day of staff time on check-in calls. Hatch gives them a way to look it up themselves, any time of day.
Secure portal access
Real time status visibility
Automatic notifications
Document hub


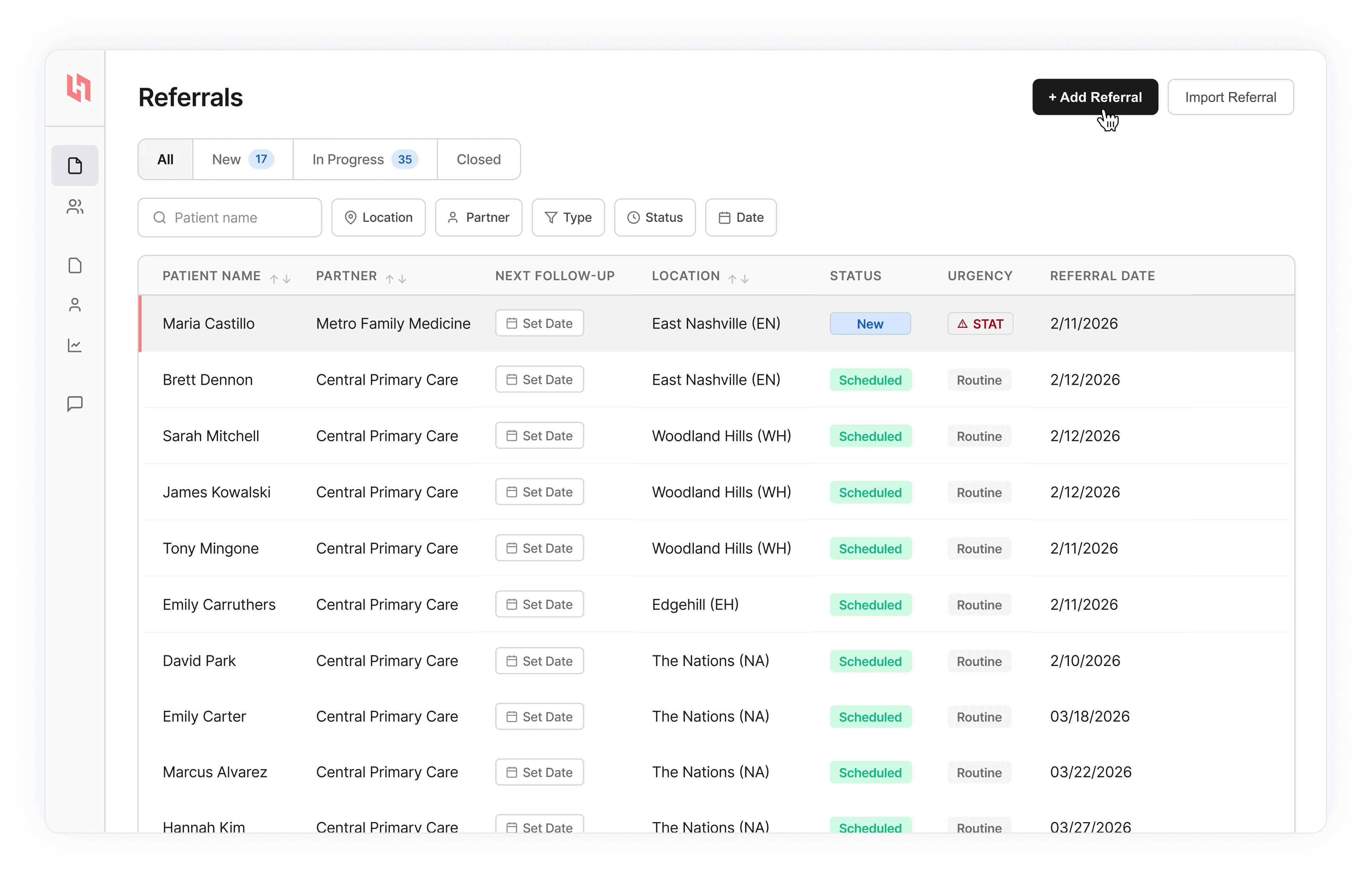
Centralized Workflows
Right now your team tracks cases across the EHR, email, fax, and spreadsheets. Hatch puts it all in one place so nothing gets lost between systems.
Centralized WC referral queue
Status tracking
Document hub
Source and partner reporting
What makes workers' comp different from general referral management in Hatch?
WC-specific intake fields, a partner portal built for adjusters and TPAs, and proactive status updates designed for multi-stakeholder communication.
Does Hatch replace our EHR?
No. Providers stay in the EMR. Hatch handles intake, communication, tracking, and the partner experience around each case.
What if our referral sources still fax or email?
Hatch handles that. Drop the document in, AI extracts the key information. As partners see the portal experience, adoption follows.
How does the partner portal work?
Adjusters get a secure, password-free link via email. They view status, access documents, and see updates without creating an account.